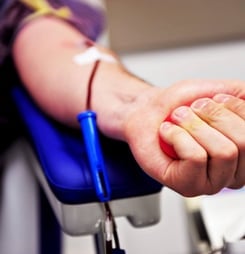
While many life-saving organ donor situations take place after the donor has deceased, in certain medical situations, it is possible for an organ to be donated by a person who is living and healthy.
National Living Donor Day seeks to improve public awareness about the possibility and process of living donors, encouraging more people to understand and be aware of how becoming a living organ donor might save the life of a friend or family member.
Living donation can sound like something out of a medical drama, but it is a carefully regulated, thoroughly evaluated practice that has helped many people avoid years of declining health while waiting for an organ.
It also comes with real responsibilities and real risks, which is exactly why education matters. This day creates space for honest conversation about what living donation is, what it is not, and how potential donors and recipients can navigate the process with clear expectations and strong support.
How to Celebrate National Living Donor Day
National Living Donor Day invites everyone to participate in a variety of ways with plans and activities. Consider some of these ideas for observing the day:
Learn Important Facts About Living Donation
One of the best ways to get involved with National Living Donor Day might be to get more informed about the process.
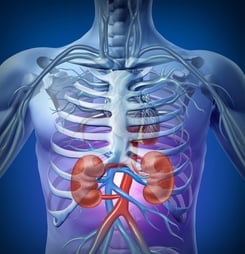
The most common living organ donation is when a person donates one of their kidneys to help someone in kidney failure and the donor is able to live normally with their one functioning kidney.
Another living donation is when a person gives a portion of their liver. When this happens, the remaining liver cells in the donor will rejuvenate and eventually grow back.
Living organ donors undergo a rigorous screening process to be sure they are a viable candidate
Many times, living donors are related to the recipient, which may cut down on rejection problems, but this is not always the case.
Consider Becoming a Kidney Donor
National Living Donor Day invites everyone to take part in different ways through thoughtful activities and simple acts of awareness. Some people observe the day quietly by learning more about living donation, while others use it as an opportunity to thank a donor, share a personal experience, or help someone understand options they may not have known about before.
What matters most is keeping the focus on informed, voluntary decisions and respect for privacy, because medical choices are deeply personal even when the outcomes can change lives.
Learn Important Facts About Living Donation
One of the most meaningful ways to participate in National Living Donor Day is by becoming better informed about how living donation works.
Living donation usually means donating an organ, or a portion of an organ, while the donor is still alive. In most transplant programs, the donor evaluation process is designed to answer two key questions: Is the procedure medically safe enough for the donor? And is the donor making this choice freely and without pressure? That second question carries just as much weight as the first.
- The most common type of living organ donation involves a person giving one of their kidneys to someone experiencing kidney failure, while the donor continues living normally with their remaining kidney.
Most individuals are born with two kidneys, but only require one to live a healthy life. After donation, the remaining kidney often adapts and increases its workload. Donors are typically encouraged to keep up with regular health care visits, including blood pressure monitoring and yearly checkups, since maintaining long-term kidney health becomes especially important. - Another form of living donation occurs when someone donates a portion of their liver. When this happens, the liver has the remarkable ability to regenerate over time.
Although this regrowth is a genuine biological process, it does not happen instantly. Liver donation involves major surgery and recovery, and it may take weeks or months for energy levels to fully return. Because the liver carries out many essential functions, transplant teams are particularly careful about selecting donors and monitoring their recovery afterward. - Living organ donors go through a detailed screening process to confirm they are suitable candidates.
Screening is rarely limited to a single appointment. It usually includes blood tests, tissue typing, imaging scans, and consultations with several medical specialists. Many transplant programs also conduct a psychosocial evaluation because factors like stress, anxiety, family relationships, and work or financial concerns can influence a donor’s experience and recovery. - In many cases, living donors are related to the recipient, which can sometimes increase the chances of compatibility, though this is not always necessary.
Family members may be good matches, but unrelated donors can also be compatible. Matching depends on specific biological factors, and transplant medicine now offers several approaches that help when a direct match is not possible.
Beyond these basics, it can also help to understand what living donation may involve and what it usually does not include.
Kidney and liver donation are the most widely recognized examples, but in certain circumstances, living donation can involve other organs or tissues, depending on medical practice and transplant center expertise.
Some people also confuse living organ donation with living tissue donation, such as bone marrow or blood stem cell donation. These are different medical procedures with different risks, though they share a common principle: a healthy individual choosing to help another person survive or regain quality of life.
National Living Donor Day is also an opportunity to address some common misconceptions:
- Living donation is never treated casually by reputable transplant programs. A donor may be declined if the medical team believes the risks are too high, even when the donor is willing.
- A donor should never feel obligated to proceed. Ethical transplant systems include safeguards that allow donors to step back. Some programs even provide ways for donors to withdraw without needing to explain their reasons to family members.
- Recovery is a real and necessary part of the process. Even with modern surgical techniques, donation remains surgery. Planning for time away from work, help at home, and emotional support is an important part of responsible preparation.
- Living donation is not risk-free for donors, and it does not guarantee a cure for recipients. Transplant teams discuss potential benefits, possible complications, and long-term expectations so everyone involved can make informed decisions.
A thoughtful way to observe the day is by reading first-person stories from donors and recipients with both compassion and curiosity. Personal experiences can be powerful, yet every situation is unique. The goal is not to replicate someone else’s journey, but to learn what questions to ask, what types of support are helpful, and what responsible transplant programs should provide.
Consider Becoming a Kidney Donor
Some people who are already registered as organ donors wonder whether that automatically means they are living donors as well. It does not. Living donation is a separate decision that requires evaluation through a transplant program.
Eligibility varies depending on the program and the individual’s health. In general, living kidney donors are adults in good overall health who can safely undergo surgery and live well with one kidney. Someone who is curious about donation can begin by learning what the evaluation process typically includes and what questions they may want to ask during an initial discussion.
Even individuals who never plan to donate can benefit from understanding the process because it helps them support someone else who may be considering it. Living kidney donation usually begins with a conversation and a preliminary health screening. If early results appear promising, the potential donor is usually guided through a more detailed evaluation that may include:
- Compatibility testing, including blood type and other biological markers
- Kidney function tests and imaging scans
- General health screenings, such as blood pressure and metabolic assessments
- A review of medical history and current medications
- A psychosocial interview to discuss motivations, support systems, and possible stress factors
Another point worth noting is that living kidney donation does not always happen between a donor and a specific friend or family member. Some transplant systems offer paired exchange programs, sometimes called swap programs. In these programs, a donor who is not compatible with their intended recipient can donate to another patient, while the original recipient receives a compatible kidney from a different donor. These exchanges can create chains that allow multiple people to receive transplants from a single series of donations.
National Living Donor Day can be observed by helping normalize conversations about living donation while keeping them respectful and realistic. Practical ways to do this might include:
- Hosting a small educational gathering with a medical professional, transplant coordinator, or trained advocate who can explain the process and answer general questions.
- Encouraging workplaces or community organizations to highlight transplant education, focusing on informed consent and support for individuals facing complex medical choices.
- Creating a personal list of questions for anyone considering donation, such as: What are the surgical risks? What does the recovery timeline look like? Who will help during recovery? What follow-up care is recommended? How are donor rights and privacy protected? What expenses are typically covered, and what costs might still arise?
It can also be meaningful to recognize and thank living donors. A simple note of appreciation, assistance with errands during recovery, or sincere acknowledgment of their decision can make a difference. At the same time, it is important to respect donors who prefer privacy and do not wish their medical decisions to become public attention.
National Living Donor Day Timeline
First Successful Living Kidney Donor Transplant
Dr. Joseph Murray and colleagues in Boston performed the first successful kidney transplant between living identical twins, proving that a healthy person can safely donate a kidney and that organ transplantation can work long term.
First Successful Living Donor Liver Transplant
Surgeons at the University of São Paulo in Brazil, led by Dr. Silvano Raia, carried out the first successful living donor liver transplant by transplanting part of a mother’s liver into her child, establishing the feasibility of partial liver donation.
National Organ Transplant Act Establishes U.S. Framework
The United States enacts the National Organ Transplant Act, creating the Organ Procurement and Transplantation Network and banning organ sales, which shapes ethical and legal protections for both deceased and living organ donors.
Introduction of Laparoscopic Donor Nephrectomy
Dr. Lloyd Ratner and a team at Johns Hopkins performed the first laparoscopic living donor nephrectomy, reducing pain, scarring, and recovery time for kidney donors and making living donation more acceptable to many volunteers.
First Reported Living Donor Liver Transplant in the United States
A team at the University of Chicago performed the first reported living donor liver transplant between adults in the United States, expanding living liver donation options beyond pediatric cases and broadening clinical experience with partial liver grafts.
Launch of the U.S. National Living Donor Assistance Center
The Health Resources and Services Administration funds the National Living Donor Assistance Center to help reimburse travel and related expenses for living donors, reducing financial barriers and encouraging altruistic donation.
First Multi‑Center Kidney Paired Donation Programs
Transplant centers in the United States and Europe began organized kidney paired donation programs, allowing incompatible donor-recipient pairs to swap kidneys with others, which greatly increases the number of transplants from living donors.
History of National Living Donor Day
The first successful living donor organ transplant took place in Boston, Massachusetts, on December 23, 1954. The operation was performed on identical twins who were 23 years old at the time.
In that historic transplant, one brother donated a healthy kidney to his twin, who was experiencing kidney failure. Both men went on to live active and healthy lives.
Over the decades that followed, significant advances in medicine have helped make transplant surgeries safer and more successful.
That early transplant is remembered not only because it succeeded, but also because it changed what medicine believed was possible. Organ transplantation faced many challenges, particularly the body’s immune system rejecting foreign tissue.
Because the transplant occurred between identical twins, the immune barrier was greatly reduced, allowing surgeons to concentrate on the surgical procedure itself. The success of this case helped stimulate further research in immunology, anti-rejection medications, and surgical techniques that would eventually expand the possibilities of transplantation.
As transplant medicine progressed, living donation developed alongside it. Several medical and technological improvements played important roles:
- Advances in imaging and diagnostic testing allowed doctors to evaluate donors more carefully and plan surgeries with greater precision.
- Improvements in anesthesia, infection control, and postoperative care reduced complications and improved recovery outcomes.
- More effective anti-rejection medications improved transplant success for recipients, which indirectly influenced living donation as well. When transplant outcomes improve, the benefits become clearer for patients and their families.
- Minimally invasive surgical techniques, especially for kidney donation in many centers, shortened hospital stays and reduced recovery times compared with older surgical approaches.
At the same time, ethical standards evolved. Transplant programs began emphasizing that living donors are patients in their own right, not simply a means of helping another patient.
This perspective led to modern safeguards such as independent donor advocates, thorough informed-consent procedures, and structured follow-up care designed to protect donor health.
National Living Donor Day was created to highlight living donation within the broader field of organ donation awareness. General campaigns about registering as an organ donor sometimes overshadow living donation, even though it involves different considerations and more immediate decisions for donors and recipients.
By focusing on education and awareness, National Living Donor Day encourages people to move beyond general goodwill toward a deeper understanding of the process. It emphasizes that living donation is not only an individual act of generosity but also a coordinated medical effort involving surgeons, nurses, transplant coordinators, social workers, mental health professionals, and the loved ones who support recovery.
The day also highlights the broader impact of living donation. For recipients, receiving an organ from a living donor can reduce waiting times and often allows transplantation before their health declines further. For donors, the experience can bring a mix of emotions.
Many report deep satisfaction and relief, while also navigating normal recovery challenges such as fatigue, temporary physical limitations, and ongoing follow-up care. A day dedicated to living donors creates space for all of these realities: gratitude, honesty, and respect for a decision that should always be informed and freely made.