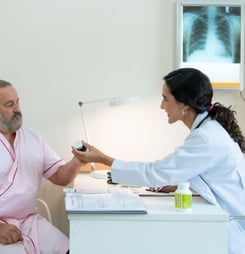
National Patient Recognition Day is a special time set aside to honor patients and highlight their importance in the healthcare system. At first glance, that might sound obvious. Of course, patients matter.
But in busy clinics, crowded waiting rooms, and fast-paced hospital units, it can be surprisingly easy for the “patient experience” to get reduced to checklists, appointment slots, and paperwork.
This observance puts the focus back where it belongs: on real people navigating real health concerns.
This day focuses on the vital role patients play, emphasizing that their experiences and satisfaction are crucial for improving healthcare services. Patients are not passive recipients of care. They provide symptoms, histories, preferences, fears, and goals.
They follow treatment plans (or do not), ask questions, notice side effects, track progress, and share what helps. When healthcare systems listen to that information, care becomes safer, clearer, and more effective.
It’s a moment for healthcare providers to reflect on the patient journey, acknowledging the strength and resilience of those they care for.
The “journey” can include everything from finding transportation to appointments, navigating insurance, waiting for test results, managing chronic pain, learning new routines, and coping with uncertainty. Recognizing patients means acknowledging not just the medical event, but the human effort wrapped around it.
Moreover, National Patient Recognition Day boosts the morale of patients and healthcare workers alike. For patients, it brings recognition and appreciation for their courage and perseverance.
Some patients feel invisible in systems that are designed for efficiency, not comfort. A sincere moment of appreciation can remind them that they are seen as individuals, not as room numbers or chart entries.
For healthcare workers, it reinforces the importance of their mission and motivates them to continue striving for excellence in patient care. When staff members hear patient feedback, thank you notes, or stories of progress, it counterbalances the emotionally heavy parts of healthcare.
Even seasoned professionals can benefit from a reminder that small actions, such as explaining a procedure carefully or returning a phone call promptly, can make a lasting difference.
This mutual appreciation fosters a stronger, more compassionate healthcare environment. It also supports a more collaborative approach, where patients feel comfortable speaking up, asking for clarification, and participating in decisions.
That kind of partnership is not just “nice.” It can reduce misunderstandings, improve follow-through, and help care teams tailor treatment to what is realistic in a patient’s everyday life.
National Patient Recognition Day Timeline
American Medical Association Code of Ethics Emphasizes Patient Interests
The newly formed AMA adopts its first Code of Medical Ethics, signaling a professional duty for physicians to place patients’ welfare and dignity at the center of medical practice.
Nuremberg Code Articulates Voluntary Informed Consent
Following World War II, the Nuremberg Code established that voluntary informed consent of human subjects is essential, profoundly influencing modern concepts of patient rights and autonomy.
World Medical Association Adopts the Declaration of Helsinki
The WMA’s Declaration of Helsinki sets ethical principles for research involving human subjects, strengthening protections for patients and emphasizing respect, informed consent, and welfare.
Canterbury v. Spence Expands Legal Duty for Informed Consent
The U.S. Court of Appeals rules that physicians must disclose material risks that a reasonable patient would want to know, shifting focus from physician-centered standards to patient-centered decision-making.
Belmont Report Defines Respect for Persons and Beneficence
The U.S. National Commission’s Belmont Report outlines core ethical principles for human subjects research—respect for persons, beneficence, and justice—reinforcing the moral basis for recognizing and protecting patients.
Patient Self-Determination Act Promotes Patient Autonomy
The U.S. Patient Self-Determination Act requires healthcare institutions receiving federal funds to inform adult patients of their rights to make decisions about their medical care, including advance directives.
Institute of Medicine’s “Crossing the Quality Chasm” Defines Patient-Centered Care
An influential IOM report identifies patient-centered care as a core aim of healthcare quality, calling for systems that respect patient preferences, needs, and values and ensure these guide all clinical decisions.
History of National Patient Recognition Day
National Patient Recognition Day began in 1995, thanks to John O’Malley. He set this day to highlight the crucial role patients play in the healthcare system. At the time, healthcare organizations were increasingly discussing service quality, patient satisfaction, and accountability.
O’Malley’s idea fit into that wider shift by encouraging facilities to treat patient perspectives as essential information rather than optional commentary.
The focus was to ensure that patient satisfaction became a top priority for healthcare providers.
Satisfaction is sometimes misunderstood as simply “making people happy,” but in healthcare it often reflects practical fundamentals: whether patients can get questions answered, whether instructions are understandable, whether pain and discomfort are addressed respectfully, and whether concerns are taken seriously.
When patients feel heard and informed, they are more likely to engage with their care and less likely to leave confused or frustrated.
This day encourages recognizing patients’ needs and valuing their input in their healthcare journey. That includes the basics, such as using clear language rather than jargon, and it also includes deeper practices, such as shared decision-making.
A patient’s values matter. One person might prioritize aggressive treatment; another might prioritize comfort, independence, or minimizing side effects. Recognition means making room for those priorities.
O’Malley’s initiative aimed to create a more patient-centered approach in healthcare. He believed that acknowledging patients’ experiences and feedback would lead to better healthcare outcomes.
Patient-centered care is now a widely used phrase, but it is built from very specific behaviors: introducing oneself, confirming preferred names, explaining delays, checking understanding, discussing options, and respecting cultural and personal context. These are small acts that add up to dignity.
By giving patients a voice and involving them in their care decisions, the healthcare system could improve its services and foster stronger patient-provider relationships.
Trust grows when people feel included. And trust is not merely a feel-good extra. It supports honest communication, which helps clinicians make more accurate assessments and helps patients raise concerns earlier, before small issues become bigger ones.
National Patient Recognition Day is now part of a broader effort to enhance patient care. It underscores the importance of patients’ perspectives and strives to make healthcare more responsive and empathetic.
Many healthcare organizations collect formal feedback through surveys, follow-up calls, and patient advisory groups. This day complements those efforts with something more personal: an intentional moment of appreciation.
This day not only honors patients but also motivates healthcare professionals to continue providing compassionate and personalized care.
Recognition can also highlight the wide range of “patients” a facility serves: children learning bravery at checkups, adults managing long-term conditions, people rehabbing after injury, and caregivers who attend visits and take notes.
When a care environment acknowledges these experiences, it creates a culture where kindness is a standard, not a bonus.
How to Celebrate National Patient Recognition Day
Celebrating this day reminds everyone involved in healthcare to prioritize patient satisfaction and engagement. It is also a chance to translate warm intentions into concrete improvements.
Appreciation is powerful, but practical support is often what patients remember most: clear signage, shorter wait times, a friendly explanation of next steps, or help coordinating care.
It encourages healthcare workers to listen more closely to their patients’ needs and concerns. Listening can be structured, not just spontaneous.
Teams might decide to ask a consistent set of questions, such as “What matters most to you about your care?” or “What part of today’s visit felt confusing?” They can also practice “teach-back,” where the patient repeats instructions in their own words to confirm understanding.
By focusing on these aspects, healthcare providers can enhance the overall experience and outcomes for patients.
Better experiences can reduce missed appointments, lower anxiety, and improve treatment adherence. For patients, feeling respected can make it easier to share sensitive symptoms, mental health concerns, or medication issues that could affect safety.
This celebration serves as a reminder of the dedication required to deliver high-quality, empathetic care. It also invites non-clinical staff into the story.
Receptionists, transport staff, lab technicians, and housekeeping teams all shape the patient experience. Recognizing patients can naturally lead to recognizing the entire ecosystem that supports them.
Shower Patients with Kind Words
Everyone loves a good compliment! Encourage healthcare providers to start the day with a smile and some kind words for their patients.
The key is to keep praise sincere and specific. Instead of a generic “You’re doing great,” staff might say, “Thank you for keeping track of your symptoms,” or “You asked important questions today,” or “I appreciate how patiently you’ve handled the delays.”
Little notes or verbal acknowledgments can make a patient’s day brighter. A short message on a bedside card, a sticky note on discharge instructions, or a printed “We’re glad you’re here” message can soften an intimidating environment.
For patients who are nervous about procedures, reassurance like “You’re not alone, we’ll talk you through each step” can be a meaningful form of recognition.
Think of it as spreading sunshine in the hallways! Kind words also help families and caregivers, who often carry stress quietly. A quick “Thanks for being here and helping” recognizes their effort, too.
Host a Mini Celebration
Why not throw a mini-party? Decorate the waiting room with balloons and streamers. Keep decorations practical and accessible, making sure signage remains visible, and walkways stay clear for mobility devices.
The goal is not a carnival vibe, but a gentle signal that the space is meant for people, not just processes.
Offer small treats like cookies or fruit to patients waiting for their appointments. Including options for common dietary needs, such as sugar-free or allergy-friendly snacks, makes the gesture welcoming rather than awkward. Even offering water, tea, or a simple refreshment station can communicate care.
Celebrating patients makes the environment more cheerful and welcoming. It can also reduce tension in waiting rooms, where uncertainty and discomfort often build.
A calmer atmosphere supports staff, too, because respectful interactions flow more easily when people feel at ease.
Share Patient Stories
Patient stories are often touching and inspiring. Create a bulletin board or a digital slideshow featuring patient testimonials. These stories can highlight successes, but they should also honor perseverance.
Not every story is about a dramatic turnaround. Sometimes it is about taking first steps after surgery, sticking with therapy, learning to manage a new diagnosis, or finding the courage to ask for help.
Sharing these stories can highlight their journeys and resilience, bringing a sense of community and support.
It can also help new patients feel less isolated. Seeing that others have faced similar fears or obstacles can be a quiet form of comfort.
When sharing stories, facilities should protect privacy and obtain clear permission. Patients can choose how much to share, whether they want names included, and what details they feel comfortable sharing. Recognition should always feel empowering, never exposing.
Create Thank You Cards
Grab some colorful paper and markers! Encourage staff and patients to create thank you cards for each other.
Patients can thank a nurse who explained a medication, a technician who made a test less scary, or a receptionist who helped reschedule after a setback. Staff can thank patients for their patience, trust, and effort.
This creative activity can foster gratitude and positive vibes throughout the healthcare facility. It can also provide a constructive outlet for feelings that are hard to express out loud. For patients who struggle with anxiety, writing can be easier than speaking.
To make it accessible, offer large-print options, simple templates, and a place to dictate a message if writing is difficult. A recognition activity works best when everyone can participate comfortably.
Offer Small Tokens of Appreciation
Give out small tokens of appreciation, like flowers, pins, or keychains. These little gifts can make patients feel valued and appreciated.
Consider items that are practical and uplifting, such as lip balm, mini hand lotion, socks with grip dots, a pocket-sized notebook for questions, or a cheerful pen for signing forms.
It’s a small gesture that can leave a big impact. The best tokens are inclusive and low-pressure. They should be offered freely, without requiring patients to share personal information or participate in activities if they do not feel up to it.
Facilities can also choose tokens that reinforce health education, such as medication trackers, hydration reminders, or simple stress-relief cards with breathing exercises. Recognition can be kind and useful at the same time.
Arrange a Relaxation Session
Everyone needs a little relaxation! Arrange for a massage therapist or yoga instructor to offer free sessions to patients.
Gentle chair massage, guided breathing, or short stretching sessions can reduce stress in a clinical setting. If in-person sessions are not feasible, a quiet room with calming audio or a short guided relaxation video can still offer a reset.
A bit of relaxation can help ease the stress of medical visits and make the day special. It can also support patients who have experienced medical trauma or fear. Small calming practices, offered respectfully, can help patients feel more in control.
When planning relaxation activities, it helps to offer choices: seated or standing, silent or guided, and always opt-in. Recognition should feel like a gift, not an assignment.
Organize a Patient Appreciation Wall
Set up a wall where patients can write down what they appreciate about their healthcare experience. Provide prompts for those who want them, such as “A staff member who made a difference,” “Something that helped me feel calmer,” or “A tip I’d share with another patient.” Include space for drawings or stickers for children.
This interactive activity allows patients to express gratitude and share positive feedback, creating a feel-good atmosphere for all. It also gives organizations real-time insight into what is working. If many notes mention clear explanations or quick lab results, that is a clue about what patients value most.
To keep it welcoming, allow anonymous notes and provide multilingual options where possible. Recognition should meet patients where they are, including those who may not be comfortable writing publicly.
Provide Extra Comfort
Make waiting areas more comfortable with extra pillows, blankets, or even a small coffee station. Comfort can also include practical upgrades: a charging station for phones, a children’s corner with quiet activities, softer lighting where appropriate, and clear signs that reduce the stress of figuring out where to go.
Creating a cozy environment shows patients that their comfort matters, making their visits a bit more pleasant. Comfort also means communication.
Posting expected wait-time updates, offering a simple explanation for delays, or providing a staff member who can answer questions can reduce frustration quickly.
For patients with sensory sensitivities or high anxiety, a few quiet seats away from the busiest area can be a thoughtful touch. Recognition does not have to be grand. Sometimes it is as simple as a comfortable chair, a warm blanket, and the feeling that someone planned for their needs.







