IUGR Awareness Day shines a light on intrauterine growth restriction (IUGR), also called fetal growth restriction, a pregnancy complication in which a baby does not grow at the expected pace in the womb.
It is a topic that can feel intensely personal for families and intensely clinical for care teams, which is exactly why a dedicated awareness day matters. It creates space for clear information, compassion, and practical support.
IUGR is not the same thing as simply having a small baby. Some babies are constitutionally small because of genetics and are otherwise healthy. IUGR, on the other hand, generally describes a growth pattern that signals a problem with the baby getting what is needed to grow, most often oxygen and nutrients.
Clinically, IUGR is frequently identified when an ultrasound estimate suggests fetal weight is below the 10th percentile for gestational age, especially when other findings point to restricted growth rather than normal smallness.
This serious issue can result from a range of causes, including problems with the placenta, the pregnant person’s health conditions, or certain infections during pregnancy. The placenta is often the main character in the story of IUGR.
It is the baby’s supply line, and when blood flow through the placenta is reduced, or the placenta is not functioning well, growth can slow. Maternal conditions that affect circulation and oxygen delivery can also play a role.
Factors such as poor nutrition, exposure to tobacco or certain substances, and chronic illnesses can increase risk, as can some fetal or chromosomal conditions. In multiple pregnancies, the challenge can be even more complex because two (or more) babies may be sharing resources.
Recognizing IUGR’s impact underscores the importance of prenatal monitoring and education about its causes and risks. Many people imagine prenatal care as a simple series of appointments, but for IUGR, those visits can become a carefully choreographed system for collecting clues.
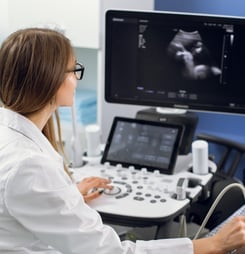
Fundal height measurements may raise the first flag when the belly measures smaller than expected. Ultrasound imaging then helps confirm whether the baby is small, whether growth is slowing over time, and whether amniotic fluid levels look normal.
Doppler ultrasound, which assesses blood flow in vessels such as the umbilical artery, can provide crucial information about how well the placenta is delivering oxygen and nutrients. In some cases, providers also use nonstress tests or biophysical profiles to assess the baby’s well-being and decide whether close observation or earlier delivery is safer.
Babies born with IUGR may face a higher risk of health challenges like delayed development and metabolic issues, particularly if they are born prematurely. In the newborn period, some IUGR babies struggle with blood sugar regulation (hypoglycemia), temperature control, feeding stamina, or higher susceptibility to infection.
If the baby is early as well as small, the risks multiply: breathing difficulties and other complications of prematurity can require specialized support. Over the longer term, some children need additional monitoring for growth patterns and developmental milestones.
Many babies with IUGR do very well, especially with timely detection and appropriate care, but the extra risk is real, and it is something families deserve to understand without being frightened into silence.
Raising awareness helps more parents and healthcare providers recognize signs of IUGR and understand potential preventive measures.
While no single strategy prevents every case, awareness supports the basics that matter: consistent prenatal care, attention to maternal health conditions, avoiding smoking and other exposures that restrict oxygen delivery, and seeking evaluation when fetal movement changes or when growth concerns arise.
It also encourages people to treat growth monitoring as meaningful medical information, not as a casual guessing game.
IUGR Awareness Day encourages community involvement, urging people to learn about the condition and support those affected, creating a network of understanding and action for better maternal and fetal health outcomes.
It also reminds everyone that complicated pregnancies are not rare side plots. They are part of real life, and families navigating them benefit from practical help and respectful listening.
How to Celebrate IUGR Awareness Day
IUGR Awareness Day offers a chance to share knowledge, support families, and strengthen community understanding around a condition that can be confusing, emotional, and medically complex.
The most helpful celebrations balance heart with accuracy: uplifting families while also sharing the kind of information that can prompt earlier care and better outcomes.
Share the Facts
Educate friends, family, or coworkers about IUGR using clear, bite-sized facts that people can actually remember. One useful place to start is the distinction between “small” and “growth restricted.” A baby can be small and healthy, but IUGR often implies a medical reason the baby is not growing as expected.
Other approachable facts include:
- IUGR is often linked to placental function and blood flow, not anything a parent “did wrong.”
- It is typically detected through growth trends over time, not a single measurement.
- Monitoring can include ultrasound estimates, amniotic fluid checks, and Doppler studies of blood flow.
When sharing online, it helps to keep posts respectful and calm. Avoid dramatic language and focus on what awareness can do: encourage prenatal appointments, help families know which questions to ask, and normalize the need for extra monitoring. The goal is not to turn a feed into a medical textbook, but to make IUGR feel less mysterious and less isolating.
Tell a Story
Personal stories often stick with people because they put real emotion and real decisions behind clinical terms. Sharing a story can mean many things: a parent describing frequent scans and anxious waiting, a partner talking about learning NICU routines, or an adult who was born with IUGR reflecting on early growth and later health.
The most supportive stories tend to include a few grounding details:
- What families wish they had known earlier (for example, what extra monitoring looked like).
- What helped emotionally (support groups, counseling, practical help at home).
- How friends and family could have shown up better (meals, childcare, listening without giving unsolicited advice).
It is also perfectly valid to tell a story that includes grief. Some IUGR journeys involve loss, and awareness should make room for remembrance as well as celebration of thriving kids.
If sharing publicly, consent and privacy matter. Families can tell their own stories without sharing medical details that feel too personal or identifying.
Host a Fun Fundraiser
Throw a bake sale, host a craft night, organize a community walk, or set up a friendly game day. Adding a playful element can make fundraising feel welcoming rather than heavy, which helps draw in people who might otherwise shy away from a medical topic.
To keep it meaningful, pair the fundraiser with a small educational piece:
- A short handout with basic definitions and why monitoring matters.
- A poster explaining what the placenta does and how it can affect growth.
- A display of “support ideas” for families who are suddenly attending frequent appointments.
Funds can be directed toward maternal and infant health initiatives, prenatal education efforts, or research programs focused on pregnancy complications and newborn outcomes. Even if the amount raised is modest, the ripple effect of awareness often outlasts the event itself.
Go Purple
Consider wearing purple for the day, a color often associated with maternal and infant health advocacy. It is simple, visual, and low-pressure, which makes it a great option for workplaces, schools, and community groups.
To make the gesture more than just a color theme, people can pair it with a conversation starter:
- “Purple for IUGR awareness. Want to know what IUGR is?”
- “Purple today to support families dealing with complicated pregnancies.”
A group photo can be a cheerful way to show solidarity, especially if it includes a short caption that defines IUGR in plain language. The idea is to create visibility without turning anyone’s medical experience into a trend.
Reach Out and Connect
Many families dealing with IUGR feel alone, particularly when their pregnancy does not match the upbeat expectations around baby showers and milestone photos. Practical support can be incredibly grounding during a time filled with scans, uncertainty, and sometimes bed rest or activity restrictions recommended by a care team.
Thoughtful ways to connect include:
- Offering rides to appointments or help with childcare for older children.
- Dropping off freezer meals or setting up a rotating meal schedule.
- Checking in with specific, easy-to-answer questions like, “Do you want company, distraction, or quiet support?”
- Supporting partners and caregivers, too, who may be juggling work, worry, and logistics.
For families whose babies spend time in a NICU, support can shift toward helping them maintain daily life: pet care, laundry, gift cards for parking or meals, or simply being the person who sends a message that does not require a reply. Small gestures can make a big impact, reminding families they are part of a wider network that cares.
IUGR Awareness Day Timeline
First reports linking low birth weight to later heart disease
British epidemiologist Richard Doll and colleagues published early data hinting that birth size may be related to later coronary heart disease, sparking interest in fetal influences on adult health.
Ultrasound biometry becomes a tool for monitoring fetal growth
Stuart Campbell and others standardize ultrasound measurements of fetal head, abdomen, and femur length, allowing clinicians to estimate fetal weight and identify fetuses that are small for gestational age.
Barker proposes the “fetal origins” of adult disease
David J. P. Barker publishes evidence from English cohorts linking low birth weight with higher adult death rates from coronary heart disease, forming the basis of the Barker hypothesis about fetal programming.
Formalization of the fetal programming concept
Barker and colleagues refine their theory that undernutrition in utero permanently alters structure and metabolism, increasing adult risk of cardiovascular and metabolic disorders, and shift research focus to fetal growth restriction.
Umbilical artery Doppler accepted for IUGR management
Clinical studies in the early 1990s show that abnormal umbilical artery Doppler waveforms in growth‑restricted fetuses predict perinatal complications, leading to guideline recommendations for Doppler in IUGR surveillance.
International consensus on fetal growth restriction terminology
Perinatal experts move from the broad label “small for gestational age” toward distinguishing constitutionally small fetuses from true intrauterine or fetal growth restriction, emphasizing blood flow and placental function.
Developmental Origins of Health and Disease is recognized as a field
The emerging DOHaD discipline integrates decades of work on IUGR, low birth weight, and chronic disease, framing growth restriction in pregnancy as a key pathway to adult cardiovascular and metabolic illness.
History of IUGR Awareness Day
IUGR Awareness Day was developed as part of a broader push to improve understanding of intrauterine growth restriction and to support those affected by it.
The day’s focus reflects a real clinical need: IUGR is not rare, and it carries meaningful risks that can be reduced when the condition is recognized early and monitored carefully.
In medical practice, concern often arises when a fetus measures smaller than expected for gestational age, especially when growth slows between ultrasounds or when blood flow studies suggest placental insufficiency.
That mix of clinical nuance and high emotion makes IUGR a condition that can be misunderstood outside obstetric and neonatal care. Awareness efforts have aimed to bridge that gap by translating medical language into everyday understanding and by encouraging people to take prenatal monitoring seriously.
Advocacy for IUGR awareness has been fueled by overlapping communities: clinicians who want better screening and clearer communication, researchers investigating placental function and long-term outcomes, and parents who have navigated intensive monitoring, early delivery decisions, NICU stays, or long follow-ups after birth.
Over time, personal storytelling has become one of the strongest engines of awareness. Families have shared what it feels like to hear that a baby is “measuring behind,” to attend frequent ultrasounds, and to live with the uncertainty of whether the safest plan is to continue the pregnancy longer or deliver early.
This public conversation has helped clarify several points that are central to the modern understanding of IUGR:
- IUGR is often about the placenta. The placenta’s ability to deliver oxygen and nutrients can change over a pregnancy, and growth restriction may be a sign that the baby is adapting to limited supply.
- Trends matter. One ultrasound can be off by a margin, but repeated measurements show whether growth is steady, slowing, or stalling.
- Monitoring is an intervention. Even when there is no “cure” to make the placenta work better, careful monitoring helps clinicians choose the safest timing of delivery and prepare the right level of newborn care.
- Outcomes vary. Some babies catch up in growth quickly. Others need longer support with feeding, temperature regulation, or developmental follow-up. Awareness messaging increasingly emphasizes this range, offering realism without assuming the worst.
While documentation about a single founder or originating organization is limited, the purpose of IUGR Awareness Day has stayed consistent: promote education, encourage early detection, and ensure families feel less alone when they hear a diagnosis that can sound frightening.
In that sense, the day is both informational and deeply human. It invites communities to learn the basics of fetal growth and prenatal care, while also recognizing the resilience of families and the importance of compassionate medical support.
Observed year after year, IUGR Awareness Day continues to encourage conversations that are easy to postpone in everyday life: how pregnancy complications can look, why prenatal visits matter, how to support someone facing complex medical decisions, and how research and clinical care can keep improving.
The broader message is simple and powerful: when a baby is not growing as expected, attention, knowledge, and coordinated care can make a meaningful difference.
Understanding IUGR: How Early Growth Shapes Lifelong Health
Intrauterine Growth Restriction (IUGR) highlights how conditions in the womb can influence both immediate survival and long-term health.
These facts explain the body’s protective responses when resources are limited, the underlying causes related to placental blood flow, and the lasting impact that restricted fetal growth can have on health later in life.
Placental “brain-sparing” blood flow is a survival strategy
When oxygen and nutrients are limited, a fetus can redistribute blood flow away from organs like the liver and toward the brain and heart, a response known as “brain-sparing.”
Doppler ultrasound studies show increased resistance in peripheral arteries and relatively preserved flow in cerebral vessels, which may help protect neurodevelopment in the short term but is also linked with higher risks of complications around birth.
Most fetal growth restriction starts with the uterine arteries
A major cause of intrauterine growth restriction is poor remodeling of the maternal spiral arteries that feed the placenta.
Instead of widening and losing their muscular layer during early pregnancy, these arteries can remain narrow and high-resistance, limiting blood flow to the placenta and chronically reducing the fetus’s oxygen and nutrient supply.
Being born small raises lifelong risks for heart and metabolic disease
Adults who were growth-restricted in the womb or born small for gestational age have higher rates of hypertension, type 2 diabetes, cardiovascular disease, and metabolic syndrome than those with average birth weights.
Large population studies and reviews suggest that poor fetal growth “programs” organs such as the pancreas, kidneys, and blood vessels in ways that make them more vulnerable to disease later in life.
IUGR alters kidney development in ways that can drive high blood pressure
Human and animal research has shown that fetuses that grow poorly tend to develop fewer nephrons, the tiny filtering units in the kidneys.
With fewer nephrons to share the workload, each unit filters more blood, which over time promotes salt retention and higher blood pressure, providing a biological link between low birth weight and adult hypertension.
Smoking in pregnancy remains one of the clearest preventable causes
Cigarette smoking during pregnancy constricts blood vessels and reduces the oxygen-carrying capacity of maternal blood, which directly impairs placental function.
Clinical guidelines consistently list smoking as a leading modifiable risk factor for intrauterine growth restriction, and quitting early in pregnancy can significantly reduce the likelihood of delivering a growth-restricted baby.
Chronic fetal hypoxia can leave a neurological footprint
When placental insufficiency limits oxygen for long periods, the developing brain can undergo structural and functional changes, particularly in white matter and regions involved in movement and cognition.
Reviews of fetal growth restriction describe higher rates of later neurologic problems, including motor difficulties and learning challenges, especially in children who were both growth restricted and born preterm.
Most small babies do not perceive a poorer quality of life as adults
Despite the increased medical risks, a follow-up study of 50‑year‑old adults who had been born with intrauterine growth restriction at term found that they reported similar health-related quality of life scores to their peers.
Using standardized questionnaires, researchers concluded that many individuals who were growth restricted in the womb adapt well psychosocially, even if their physical health risks remain elevated.